Anatomy Passions: The Temporomandibular Joint
Nov 28, 2025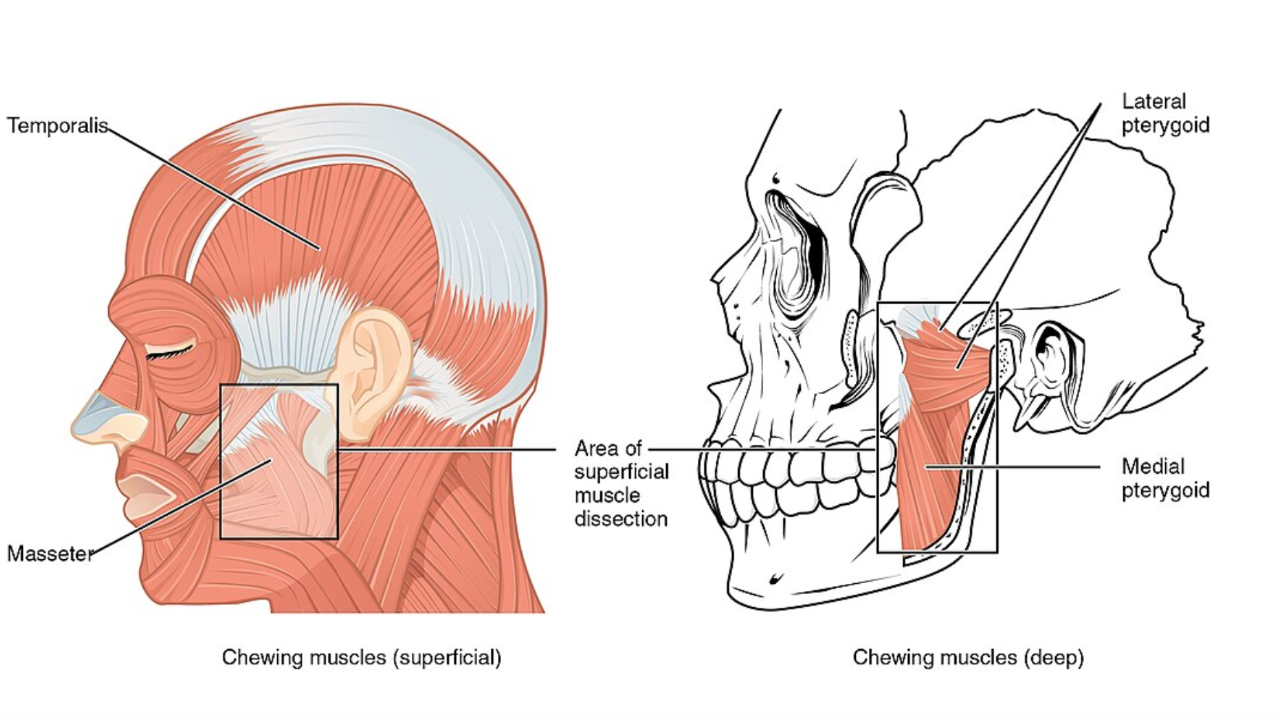
Discovering the Fascinating World of the TMJ
When it comes to a passion for body work, few people can say they’ve spent nearly 45 years exploring one area of the body in depth. For me, that area is the temporomandibular joint (TMJ)—a small but incredibly important joint that plays a role in many aspects of body movement and comfort.
Some might consider it a narrow focus, but the more I investigated this joint, the more I realized it is involved in a wide range of musculoskeletal and functional processes.
Research dating back to 1987, based on 30 years of study, highlighted connections between TMJ function and conditions as varied as headaches, back discomfort, and skin conditions such as psoriasis (1). Since then, many scientific studies have explored how the TMJ relates to sports performance (2), fibromyalgia (3), sleep quality (4,5), and brain health (6).
In one of my free CPD trainings, we discuss the glymphatic system, a recent discovery in human physiology that links aging, sleep, cardiovascular health, and brain function. The glymphatic system plays a key role in clearing waste products from the brain, which research shows are associated with conditions such as Alzheimer’s disease (7). Sleep quality can influence glymphatic function, and factors affecting sleep—such as jaw and TMJ function—may be connected to broader physiological processes (8).
A Journey of Learning
My personal journey began over 25 years ago when I trained in massage, anatomy, and physiology. At the time, the TMJ was barely mentioned in standard training. With prior experience as a dental nurse, I had already worked with patients experiencing jaw-related issues. Inspired by trigger point therapy techniques, I developed a protocol aimed at supporting people exploring comfort and function in the jaw and surrounding areas. With the consent of patients who chose to try this approach, this protocol became the foundation of TMJ Therapy®️, and has remained a key focus of my professional work ever since.
Over the years, feedback from students and clients, alongside further training in myofascial bodywork and texts such as Anatomy Trains, specifically the Deep Front Line, helped me understand the TMJ’s subtle influence on posture, movement, and overall body alignment. Some individuals have reported noticing improvements in posture or comfort after TMJ-focused work, though experiences vary and are not guaranteed.
Anatomy of the TMJ
The temporomandibular joint is widely considered the only joint in the human body that effectively crosses the midline. There are two TMJs, one on each side of the head, located just in front of the ears and linked by the single fused mandibular bone. The TMJs connect the mandible (lower jaw) to the temporal bone of the skull.
Because the two joints are connected by this single bone, they must operate in harmony and cannot move independently. Movement in one joint influences the other, meaning their function crosses the body’s sagittal midline. Unlike simple hinge joints, the TMJ combines both hinging and sliding motions, allowing the jaw to move up and down, side to side, and forward and backward.
Muscles of Mastication
The four primary muscles of mastication are the masseter, temporalis, medial pterygoid, and lateral pterygoid. These muscles are responsible for chewing and jaw movements, including closing, opening, and side-to-side grinding of food:
Masseter: Elevates the mandible to close the mouth.
Temporalis: Elevates and retracts the jaw.
Medial Pterygoid: Works with the masseter to close the jaw.
Lateral Pterygoid: Assists in opening the jaw by moving it forward and downward.
All muscles of mastication are innervated by motor fibers of the mandibular branch of the trigeminal nerve (CN V3) and receive arterial supply from branches of the maxillary artery.
Learn More in Our Free Training
If you’d like to explore this fascinating area of anatomy further, I’m running a free training in January called Ageing Well: Brain Health, Balance, and TMJD. This session will explore TMJ function, posture, balance, and overall wellbeing. Register for free here: TMJ Multi-Day Training
References
Fonder AC. The dental distress syndrome quantified. Basal Facts. 1987;9(4):141-67.
Haughey JP, Fine P. Effects of the lower jaw position on athletic performance of elite athletes. BMJ Open Sport & Exercise Medicine. 2020;6:e000886.
Sahbaz T, Karacay BC. Investigation of temporomandibular disorders in patients with fibromyalgia syndrome: A case-control study. J Stomatol Oral Maxillofac Surg. 2023.
Sanders AE, et al. Sleep apnea symptoms and risk of temporomandibular disorder: OPPERA cohort. J Dent Res. 2013;92(7 Suppl):70S-7S.
Lee YH, et al. Poorer sleep quality in patients with chronic temporomandibular disorders compared to healthy controls. BMC Musculoskelet Disord. 2022;23:246.
Corbali O, Levey AI. Glymphatic system in neurological disorders and implications for brain health. Front Neurol. 2025;16:1543725.
NIA – Alzheimer’s Disease Risk Factors
Patil K, et al. Sleep apnea and orofacial pain: an integrative clinical perspective. J Oral Facial Pain Headache. 2025;39(3):50-55.
Image Credit: OpenStax, CC BY 4.0 <https://creativecommons.org/licenses/by/4.0>, via Wikimedia Commons


